Mpox in Cameroon: 5 Confirmed Cases
A new outbreak of Mpox, commonly known as monkeypox, has been recorded in Cameroon, raising renewed concerns about the spread of infectious diseases in the country. According to the Journal du Cameroun, five confirmed cases were detected between November 14, 2025, and January 7, 2026.
This resurgence comes at a time when health authorities are already facing multiple public health challenges, including malaria, cholera, and other communicable diseases.Out of the five confirmed cases, four were reported in the Littoral Region, specifically in the health districts of Abo, Deido, and Cité des Palmiers, all located in the city of Douala. The fifth case was recorded in the South-West Region, in the Akwaya Health District, an area known for its geographical isolation and limited access to healthcare services. The concentration of cases in urban areas such as Douala is particularly worrying, as high population density increases the risk of rapid transmission.
Despite the seriousness of the situation, no deaths have been reported so far. Since the beginning of 2025, ten cases have been confirmed nationwide, and fourteen others remain suspected, according to data released by health authorities. This suggests that Mpox continues to circulate at a low but persistent level within the population.
Mpox is a viral disease caused by the monkeypox virus, which belongs to the same family as the smallpox virus. Although Mpox is generally less severe than smallpox, it can still cause significant illness, especially among vulnerable populations such as children, pregnant women, and people with weakened immune systems.
The disease is transmitted through close contact with infected individuals, animals, or contaminated materials. This includes direct skin-to-skin contact, exposure to respiratory droplets, and contact with bodily fluids or lesions. In some cases, the virus can also spread through shared clothing, bedding, or personal items. Mpox typically begins with flu-like symptoms such as fever, headache, muscle pain, back pain, and fatigue. Swollen lymph nodes are also a common feature, which helps distinguish Mpox from other similar illnesses like chickenpox.
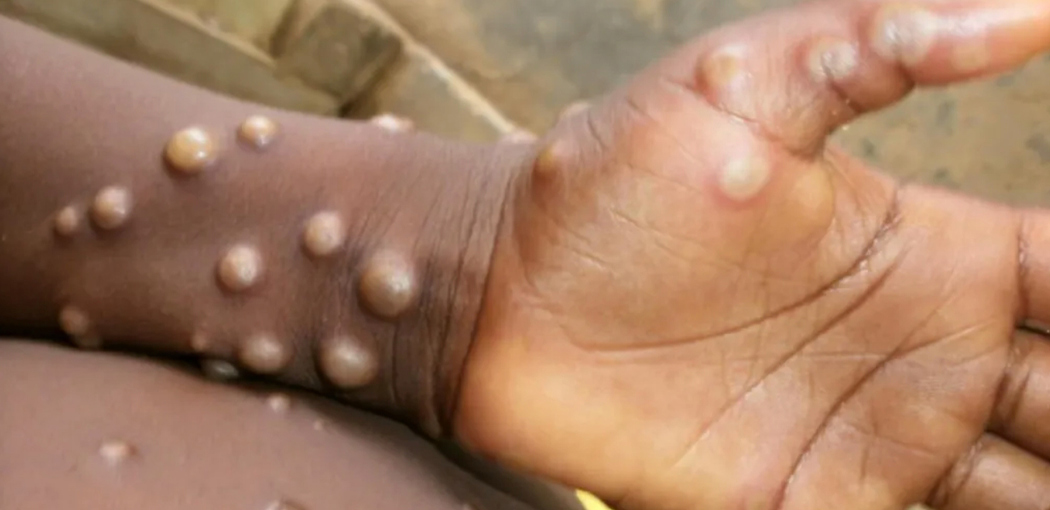
After a few days, a characteristic skin rash develops. The rash often starts on the face before spreading to other parts of the body, including the hands, feet, and genitals. The lesions go through several stages, from flat spots to fluid-filled blisters, before eventually forming scabs and healing. Health authorities recommend that anyone experiencing these symptoms should seek medical attention promptly. Early diagnosis and isolation are essential to prevent further transmission.
In response to the resurgence of Mpox, the Minister of Public Health, Dr. Manaouda Malachie, ordered the activation of an incident management system. This system aims to improve coordination between national and regional health services, strengthen epidemiological surveillance, and ensure rapid response to new cases. One of the key objectives is to improve case detection through active surveillance in health facilities and communities. Healthcare workers have been instructed to report suspected cases immediately and follow strict infection prevention and control measures.
Contact tracing has also been intensified. This involves identifying people who may have been exposed to confirmed cases and monitoring them for symptoms over a defined period. Early detection of secondary cases helps break the chain of transmission. Public awareness campaigns have been intensified, particularly in urban areas of the Littoral Region, where most cases have been reported. These campaigns aim to educate the population about how Mpox spreads, how to recognize its symptoms, and how to protect themselves and their families.
Information is being shared through radio programs, social media, community meetings, and health outreach activities. Messages emphasize the importance of good hygiene practices, such as regular handwashing, avoiding close contact with sick individuals, and seeking medical care when symptoms appear. Community leaders and local organizations play a crucial role in spreading accurate information and combating misinformation. In many areas, traditional beliefs and rumors can delay health-seeking behavior, making public education even more important.
The detection of a case in Akwaya, in the South-West Region, highlights the challenges of managing infectious diseases in remote and hard-to-reach areas. Akwaya is located far from major urban centers, with limited road access and scarce healthcare infrastructure.
In such settings, delays in diagnosis and treatment are more likely. Limited laboratory capacity, shortage of trained healthcare workers, and difficulties in transporting samples can hinder effective surveillance.To address these challenges, health authorities are working to strengthen regional health systems by providing additional training, equipment, and logistical support. Mobile health teams are also being deployed to improve access to care in underserved communities.
Mpox is not only a national concern for Cameroon but also a regional and global public health issue. Several African countries continue to report cases, and sporadic outbreaks have been recorded in other parts of the world in recent years.
The World Health Organization (WHO) has emphasized the importance of early detection, transparent reporting, and international cooperation in controlling the spread of Mpox. Surveillance systems, laboratory networks, and data-sharing mechanisms are essential tools in the global response.
Cameroon’s health authorities are working in collaboration with international partners to strengthen their preparedness and response capacity. This includes improving laboratory diagnostics, training healthcare workers, and updating national response plans.
Health services are calling for collective vigilance, respect for hygiene rules, and public cooperation to limit the spread of the disease throughout the country. The success of any outbreak response depends not only on government action but also on individual behavior.Citizens are encouraged to report suspected cases, follow health advice, and avoid spreading rumors or false information. Responsible communication helps build trust between communities and health authorities, which is essential during public health emergencies.
Although the current number of Mpox cases remains relatively low, the situation serves as a reminder of the constant threat posed by infectious diseases. Urbanization, population mobility, and environmental changes increase the risk of outbreaks. Strengthening disease surveillance, improving healthcare access, and investing in public health education are critical steps for Cameroon’s long-term health security. The Mpox outbreak highlights the importance of preparedness, rapid response, and community involvement in protecting public health.
As authorities continue to monitor the situation closely, the population is urged to remain alert, informed, and cooperative. With sustained efforts, the spread of Mpox can be contained, and future outbreaks can be managed more effectively.
